Are Sleeping Disorders Genetic? Unraveling The Mysteries
Yes, sleeping disorders can have a genetic component. Some sleep disorders, such as narcolepsy, have been linked to specific genetic mutations.
While genetics may play a role in the development of sleep disorders, it's important to note that not everyone with a genetic predisposition will develop a sleep disorder. Other disorders, such as insomnia or sleep apnea, may be more complex and involve a combination of genetic, environmental, and lifestyle factors.
- Narcolepsy
- Familial advanced sleep phase syndrome (FASPS)
- Restless legs syndrome (RLS)
- Sleep apnea
- Obstructive Sleep Apnea Syndrome (OSAS)
- Fatal Familial Insomnia
Everyone needs to sleep several hours daily to stay healthy, process information, and to re-energize. For some people, unfortunately, sleep is elusive. Approximately one-third of people around the world suffer from some kind of sleeping disorder[1]. Are these conditions genetic? Can you blame your parents for your sleep troubles?
What Are Sleeping Disorders?
Sleeping disorders are medically defined as conditions that disrupt the quality or quantity of sleep. Over 80 different sleeping disorders have been identified, including insomnia, sleep apnea, and narcolepsy[2]. Insomnia disorder is the most common type of sleeping disorder, affecting about 30% of adults worldwide[3]. `
Helpful Tip
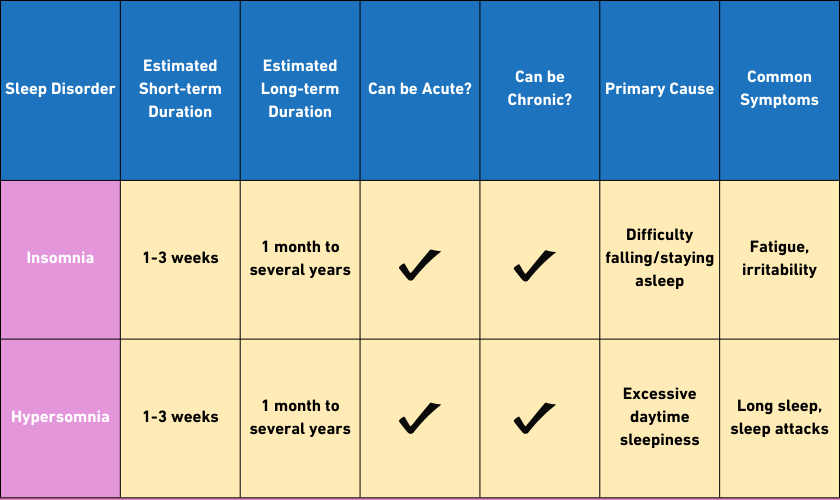
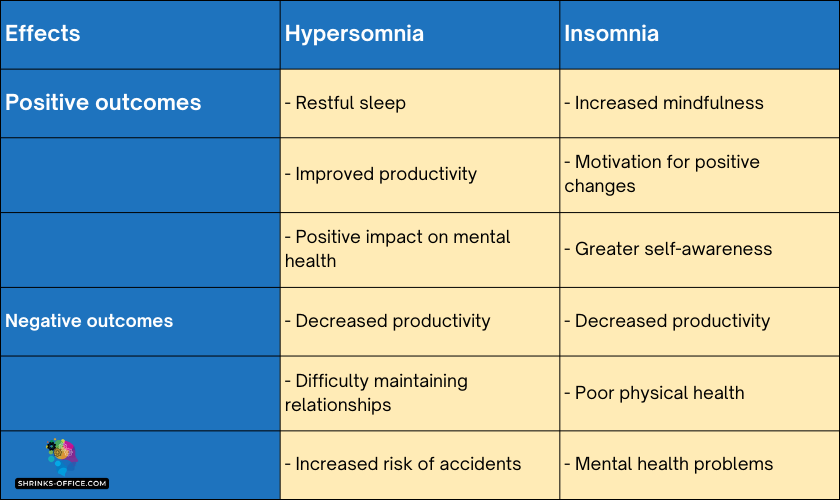
Struggling with sleep? Remember, Hypersomnia and Insomnia require different approaches. Quality sleep hygiene practices are key for both.

Understanding the Sleep Cycle: The Interplay of REM and Non-REM Sleep
Sleep isn't a single, uniform state of rest that descends upon us each night. Rather, it's a dynamic process involving different stages that cycle several times throughout the night. These stages include both Rapid Eye Movement (REM) sleep and non-REM sleep, each with its own distinctive characteristics and roles in maintaining our health and well-being.
Non-REM Sleep: The Foundation of Rest
Non-REM sleep, also known as NREM sleep, is divided into three stages:
Stage 1 (N1): This is the transition period between wakefulness and sleep, lasting only about 5-10 minutes. It's characterized by slow eye movement and a reduction in heart rate, breathing, and brain activity.
Stage 2 (N2): This stage represents the onset of sleep as we become unaware of our surroundings. Our heart rate and body temperature decrease further, and brain waves slow with only occasional bursts of rapid activity.
Stage 3 (N3): Also known as deep sleep or slow-wave sleep, this stage is vital for physical renewal and rejuvenation. During N3, growth hormone is released, aiding in cellular repair and growth. Additionally, this is the stage that helps boost immune function and manage stress and anxiety.
REM Sleep: The Dream Centre
Following the three stages of non-REM sleep, we enter REM sleep, typically about 90 minutes after falling asleep. REM sleep is when most dreaming occurs, and our brains become more active, almost akin to when we're awake.
During REM sleep, our eyes move rapidly behind our eyelids (hence the name), and our bodies become temporarily paralyzed to prevent us from acting out our dreams. This stage is crucial for memory consolidation, learning, and mood regulation.
The Sleep Cycle: A Nightly Journey
Throughout the night, we cycle through all these stages of non-REM and REM sleep several times, with each complete cycle lasting about 90 to 110 minutes. It's important to note that the duration of each stage changes throughout the night. Non-REM sleep, especially the restorative N3 stage, dominates the early cycles. As the night progresses, REM sleep periods become longer, peaking in the hours close to waking.
The Impact of Sleep Deprivation on Health
Insufficient sleep or disruptions to the sleep cycle can lead to sleep deprivation, which affects both our physical and mental health.
Physical Health Consequences
Impaired Immune Function: Chronic sleep deprivation can weaken the immune system, making us more susceptible to infections.
Increased Risk of Chronic Conditions: Lack of adequate sleep has been associated with a higher risk of various health conditions, including heart disease, diabetes, and obesity.
Negatively Impacts Growth and Development: During deep sleep (N3 stage of non-REM sleep), the body releases growth hormone. Sleep deprivation can impact this process, particularly in children and adolescents.
Mental Health Consequences
Cognitive Impairment: Sleep deprivation can affect various cognitive functions, including attention, decision-making, creativity, and memory.
Emotional and Mood Disorders: Lack of sleep can lead to mood swings, increased irritability, anxiety, and a higher risk of depression.
Reduced Quality of Life: Chronic sleep deprivation can affect one's overall well-being and life satisfaction.
Achieving a better understanding of our sleep cycle and the importance of both REM and non-REM sleep stages can be the first step in improving our sleep quality and, by extension, our health. If you're struggling with sleep, it might be beneficial to consult with a sleep specialist or a healthcare professional who can provide guidance based on your specific circumstances and needs. [5]
Did you know? Certain hormones that cause anxiety can disrupt your sleep. Balanced nutrition and relaxation techniques can help manage them.

Common Misconceptions About Sleep
There's a wealth of misinformation circulating about sleep. Here are some common misconceptions that you should be aware of:
- "I can make up for lost sleep during the week by sleeping more on the weekends." While extra sleep can help to a degree, it cannot fully make up for the effects of sleep deprivation. Regular, consistent sleep is key.
- "Snoring is a normal part of sleep." While snoring can be harmless, it can also be a symptom of a serious sleep disorder called sleep apnea, which is characterized by pauses in breathing during sleep.
- "The older I get, the fewer hours of sleep I need." While sleep patterns change as we age, the amount of sleep we need generally does not. Adults should aim for 7-9 hours of sleep per night. [5]
Are Sleeping Disorders Genetic?

According to studies, sleep is a genetically controlled behavior. Studies have shown that certain genetic variations are linked to individual sleep needs and preferences. Some of these variations are associated with the regulation of circadian rhythms, while others are associated with sleep architecture or the structure of sleep[4].
The same studies have also pointed out that certain sleeping disorders – like narcolepsy and insomnia – are linked to specific genetic abnormalities. However, the same sleeping disorder can have other non-generic factors that influence its onset and progression, which are explained below.
Genetic Sleeping Disorders

There are several sleeping disorders identified to have genetic factors as the cause of their development.
Circadian Rhythm Disorders - Generic conditions like Smith-Magenis syndrome and familial advanced sleep-phase syndrome (FASPS) are linked to genetic factors. These disorders often affect the sleep-wake cycle, causing people to either have difficulty sleeping or feel sleepy during the day.
Narcolepsy - People with narcolepsy experience daytime sleepiness, hallucinations at sleep onset, cataplexy (or sudden paralysis), and disturbed nighttime sleep. Genetic research has found that narcolepsy is caused by a combination of several genes, including HLA-DQB1, T-cell receptor alpha (TCRA), and P2RY11.[4]
Restless Leg Syndrome - RLS is a disorder that causes an urge to move the legs, especially when lying down or sitting for long periods of time, that will affect sleep quality and duration. Recent studies have identified a number of genetic markers associated with the disorder, including ones located on chromosomes 12 and 14.[4]
Obstructive Sleep Apnea Syndrome - OSAS occurs when the throat muscles relax and block your airway while you are asleep. This sleep disorder can cause trouble sleeping and are linked to high blood pressure, diabetes, asthma and excess weight. The most commonly identified genetic causes of ASAS are mutations in the PHOX2B gene and the TSHZ3 gene.
Chronic Insomnia - This is a condition that involves difficulty falling asleep or staying asleep for an extended period of time. According to sleep research, chronic insomnia is common in individuals with Morvan's syndrome and in monozygotic twins. [4]
Fatal Familial Insomnia - This is an incredibly rare condition that runs in families and is caused by mutations in a prion protein gene known as the PRNP gene. Fatal Familial Insomnia symptoms include sleep problems, weight loss, dysfunction of the autonomic nervous system, hallucinations, and eventually death. Treatment options for this disorder are limited.
Hypersomnia- Certain genetic conditions, such as Kleine-Levin syndrome and Prader-Willi syndrome, can cause Hypersomnia (excessive daytime sleepiness). People with this condition experience excessive fatigue, sleep issues, and difficulty concentrating during the day.
Parasomnia - Parasomnia conditions such as sleepwalking, talking in your sleep, bed-wetting, teeth grinding, and night terrors are all associated with genetic factors. These conditions are prevalent in children and can cause poor sleep quality and disrupted sleep patterns, leading to daytime fatigue.
Other Contributing Factors
According to MedlinePlus, there are several other contributing factors to sleep disorders besides genetics. These include[2],
- Medical conditions such as lung disease, heart disease, nerve disorders, and pain
- Certain medicines
- Mental illnesses, including depression and anxiety
- Lifestyle habits such as caffeine, drugs, and alcohol usage
- Aging
- Irregular sleep schedule, such as working the night shift
Can You Blame Your Parents for Your Sleep Troubles?
As you can see, there are other causes that can lead to sleep disorders. This means that genetics isn't the only factor to blame. While it's true that family history may contribute, you can not put all the blame on your parents.
So, if you experience any sleep problems, it is better to consult with a doctor before jumping to any conclusions.
Interesting tip
Caring for mentally ill parents can be taxing. Prioritize good sleep to maintain your own mental health and resilience in challenging times.
Diagnosis and Treatment

Diagnosis of sleeping disorders is made after a thorough physical and psychological evaluation. The doctor would also review your medical history, how much sleep you get, and your lifestyle habits, as well as any medications that you might be taking.
A sleep study or polysomnogram may also be performed to determine the frequency, duration, and quality of your sleep.
Treatments for sleeping disorders include therapies such as cognitive behavioral therapy, practicing good sleep hygiene, sleep medicine, and lifestyle changes.
How To Create a Sleep-Friendly Environment
The quality of our sleep is often directly connected to our physical environment and our lifestyle habits. For those who are struggling with sleep disorders or simply want to enhance their nightly rest, maintaining a regular sleep schedule, crafting a relaxing bedtime routine, and designing a sleep-friendly bedroom environment can be significantly beneficial. Let's delve into these areas more deeply.
Maintaining a Regular Sleep Schedule
Our bodies thrive on regularity. Establishing a consistent sleep schedule—going to bed and waking up at the same time each day—can greatly improve the quality of our sleep. This regularity helps to set our body's internal clock, or circadian rhythm, leading to more restful and restorative sleep.
Key tips for maintaining a regular sleep schedule include:
- Set Fixed Bedtimes and Wake-up Times: Aim to go to bed and wake up at the same time every day, even on weekends. This consistency helps regulate your body's clock and could help you fall asleep and stay asleep for the night.
- Avoid Long Naps: If you must nap, try to keep it short and avoid napping late in the day.
- Manage Your Exposure to Light: Exposure to natural light during the day and darkness at night helps to keep your circadian rhythms in check. Avoid bright screens for an hour before bedtime. [7]
Helpful tip: Embrace the benefits of therapy for better sleep. Discussing your anxieties can lower stress levels, leading to more peaceful and restful nights.
Crafting a Relaxing Bedtime Routine
A soothing pre-sleep routine can signal your body that it's time to wind down and prepare for sleep.
Consider these activities for your bedtime routine:
- Unplug from Electronic Devices: The blue light emitted by screens can interfere with your ability to fall asleep. Try to turn off all screens at least an hour before bed.
- Practice a Relaxation Technique: Techniques like deep breathing, meditation, progressive muscle relaxation, or visualization can help you relax and prepare your body for sleep.
- Read a Book: Reading can be a great way to unwind, just make sure it's something calming and not too engrossing.
- Listen to Soft Music or White Noise: Soft music or sounds can help create a peaceful environment conducive to sleep.

Designing a Sleep-Friendly Bedroom Environment
Your bedroom should be a sanctuary dedicated to sleep. The environment can have a big impact on the quality of your sleep.
Below are a few suggestions for designing a sleep-friendly bedroom:
- Keep It Cool, Dark, and Quiet: These conditions are ideal for sleep. Consider using earplugs or a white noise machine to block out noise, and eye shades or dark curtains to block out light.
- Invest in a Comfortable Mattress and Pillows: Ensure your bed and pillows are comfortable and supportive. The lifespan of a quality mattress is about 9 or 10 years.
- Keep Your Bedroom Tidy: A clean and uncluttered bedroom can help promote a better sleep environment.
- Limit Bedroom Activities: Use your bed only for sleep and intimacy to strengthen the association between bed and sleep. [7] [8]
Triumph Over Sleep: Personal Journeys to Restful Nights
Frida Rångtell
In the past, she didn't prioritize her sleep, often staying up late for work or leisure. However, her perspective on sleep underwent a significant shift upon becoming a mother. Her sleep became more fragmented due to her newborn's frequent wake-up calls, leading to increased fatigue. However, as her daughter grew older and began sleeping through the night, she managed to establish a better sleep routine. Her previous habit of sleeping late on weekends transformed into early mornings spent engaging with her child.
She was aware that newborns have an unstable circadian rhythm and wake up frequently for feeding and security, yet she didn't anticipate her own irritability when being awakened during the night. The experience of parenthood has taught her to adapt and make changes, particularly in regards to sleep. Now, she prioritizes sleep over personal time when her child is asleep.
She emphasizes the importance of exposure to daylight for both her and her child to maintain a healthy circadian rhythm, and avoids electronic devices during the night to ensure better sleep quality. Parenthood has not only transformed her sleep habits but also led to a newfound appreciation for the importance of a good night's sleep. [9]
Delphine Sherwood
In 2006, her life took a drastic turn as her first marriage ended, sparking a series of sleepless nights filled with intense questioning and self-doubt. She found herself waking up at 3 a.m. consistently, her sleep disturbed by vivid dreams and racing thoughts. Living in Sri Lanka at the time as a humanitarian worker, her life became a whirlwind of changes as she relocated to different states and countries over the next 13 years.
She encountered numerous personal losses, including the death of her father, her mother's cancer diagnosis, failed relationships, and unsuccessful pregnancies. All these events seemed to affirm her belief that she would forever be deprived of restful sleep, and she resigned to the impact it had on her energy levels, concentration, mood, and physical health.
However, in 2019, a surprising shift occurred. Despite enduring another challenging year marked by depression, weight gain, surgery, job loss, a divorce, and yet another relocation, she found that deep sleep had returned to her. The previously dreaded 3 a.m. mark was either bypassed or, if woken, she could quickly return to sleep. Now in a new city, with a new job, single, financially strapped, and solely responsible for her three dogs, it was as if sleep had re-emerged as a peace offering amid the uncertainty.
Now, she cherishes the restful nights spent with her dogs, confident that sleep would heal the day's mishaps and quiet the endless inner chatter. Awaking refreshed and filled with a renewed sense of hope, she believes that everything will eventually be alright. [10]
Conclusion
Certain sleeping disorders can be generic or can develop over time due to one's lifestyle and environment. If one of your family members has a sleeping disorder, there is an increased chance that you might get it as well. Therefore, get screened periodically and practice good sleep hygiene to prevent the development of a sleeping disorder.
If you're struggling to sleep - Experience the transformative power of online therapy, your gateway to more peaceful nights and better sleep, all from the comfort of home.
FAQ
At what age do sleeping disorders start?
Sleeping disorders may start at any age, but they are more common in adults and the elderly.
Is insomnia inherited from the mother?
Insomnia can be inherited from either parent, but genetic predisposition is more likely to be passed on from the mother. But genetics isn't the only factor that can influence the development of insomnia. It also depends on various factors, such as environmental factors and one's lifestyle.
References
- A Review on Genetics of Sleep Disorders - PMC
- Sleep Disorders | MedlinePlus
- Sleep epidemiology—a rapidly growing field | International Journal of Epidemiology | Oxford Academic
- Genetics of Sleep and Sleep Disorders - ScienceDirect
- Molecular Autism: Sleep disorders in rare genetic syndromes
- NLM: Sleep myths: An expert-led study to identify false beliefs about sleep that impinge upon population sleep health practices
- Choc's Children: Sleep Hygiene for Teens
- Pubmed: YOUR GUIDE TO Healthy Sleep
- Sleepy Cycle: Motherhood & sleep
- Sleepy Cycle: Sleeper, interrupted